LEPTIN, STAT3, AND CANCER
In 2015 State Key Laboratory of Oncogenes and Related Genes, Shanghai
Cancer Institute, Renji Hospital, Shanghai Jiao Tong University School
of Medicine, Shanghai, China were able to us that:
"Emerging evidence has suggested that leptin, an adipokine
related to energy homeostasis, plays a role in cancer growth and
metastasis."
They explain that "Leptin up-regulated the expression of matrix
metalloproteinase-13 (MMP-13) via the JAK2/STAT3 signaling pathway.
The overexpression of leptin was shown to significantly promote tumor
growth and lymph node metastasis in a subcutaneous model and an
orthotopic model of human pancreatic cancer, respectively.
Furthermore, in human pancreatic cancer tissues, the expression of
[leptin's functional receptor] Ob-Rb was positively correlated with
the MMP-13 level."
Leptin up means metastasis up:
"Consistently, we also found the association of MMP-13
expression with lymph node metastasis and the pathological
stage"
and
"Human MMP-13, also known as collagenase-3, is a matrix
metalloproteinase originally identified in breast carcinomas. Recent
studies have revealed that this enzyme is also produced by a variety
of malignant tumors, including head and neck, breast and colorectal
cancer. In all of the cases, the expression of MMP-13 is associated
with aggressive tumors."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4599260/
[426]
Obviously I do not want leptin to be too high or too low. But people
have been regulating leptin with and without marijuana for thousands
of years before 1994.
Its novelty means the current idea of a "normal" range has
been obtained entirely during last 27 years of the unusually wealthy
recent anthropocene.
It is increased by the carbohydrates which have replaced the
hunter-gatherer diets with which early homo sapiens evolved. This
trend is discussed in considerable detail here:
https://bmcendocrdisord.biomedcentral.com/articles/10.1186/1472-6823-5-10#Sec9
[427]
Hugh J Freeman of Vancouver University:
"Celiac disease may have developed as a distinct disorder with
the transition of hunter-gatherer groups into human workforces capable
of agriculture. This "Neolithic revolution" is believed to
have permitted competitive survival over other hunter-gatherer groups
owing to more secure food supplies. Over time, celiac disease has
emerged as a major clinical disorder, currently thought on the basis
of serological studies to affect up to about 2% of most
genetically-predisposed human populations."
Celiac keeps popping up in areas of wheat consumption, faster than
could be accounted for by genetic factors.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4282854/
[428]
Battista et al, in their paper "Altered Expression of Type-1 and
Type-2 Cannabinoid Receptors in Celiac Disease" (2013)
investigated CBR mRNA and protein as well as functional activity
levels in the duodenal mucosa of UCD and TCD patients, and CS, and
say:
"Our in vivo data showed that mRNA and protein levels of both
CB1 and CB2 receptors are remarkably increased in UCD mucosa compared
to TCD mucosa and normal mucosa. It is noteworthy that in TCD patients
CB2, but not CB1, levels were reverted to normal values, pointing to
CB2 rather than CB1 as main molecular target in celiac disease.
Moreover, ex vivo experiments on organ culture confirmed that
gluten-induced damage is responsible for this increase, at least at
the protein level."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3631143/
[429]
It became clear by 2010 that The endocannabinoid system links gut
microbiota to adipogenesis, and "that macrophage infiltration is
not only dependent on the activation of the receptor CD14 by
lipopolysaccharide, but is also dependent on the gut microbiota
composition and the gut barrier function (gut permeability). Moreover,
LPS controls the synthesis of eCBs both in vivo and in vitro through
mechanisms dependent of the LPS receptor signalling pathway. Thus,
obesity is nowadays associated with changes in gut microbiota and a
higher endocannabinoid system tone, both having a function in the
disease's pathophysiology." [Fig. 2, see ecb controls
gut]
"in vivo experiments strongly suggest that an overactive eCB
system increases gut permeability."
"we measured AEA levels and FAAH [Fatty acid amide hydrolase, an
enzyme that breaks down anandamide] mRNA expression in adipose tissue.
Prebiotics strongly decreased AEA levels and tended to increase FAAH
mRNA levels (Figure 6C), further supporting the link between changes
in gut microbiota and modulation of the eCB system."
"Blocking the CB1 receptor in obese mice also ameliorated gut
barrier function as shown by improved distribution....CB1 activation
increased gut permeability markers in vivo and in vitro. This
demonstration that CB1 receptors control gut permeability suggests a
new eCB system-dependent mechanism in the pathogenesis of
obesity-associated inflammation (systemic and hepatic)."

"eCB system-LPS crosstalk participates in the regulation of
adipogenesis by gut microbiota. Activation of the eCB system in the
intestine (e.g. through gut microbiota) increases gut permeability,
which enhances plasma LPS levels. This exacerbates gut barrier
disruption and peripheral eCB system tone in both the intestine and
adipose tissues. Increased fat mass results in enhanced eCB system
tone. LPS inhibits both PPAR-induced and cannabinoid ligand-induced
adipogenesis. Overall, the impairment of these regulatory loops within
colon and adipose tissues found in obesity perpetuates the initial
disequilibrium, leading to a vicious cycle. This cycle maintains the
increased gut permeability, eCB system tone, adipogenesis and fat mass
development that characterise obesity."
"it is clear that genetic or pharmacological blockade of the CB1
cannabinoid receptor protects against the development of
obesity"
https://www.embopress.org/doi/full/10.1038/msb.2010.46
[430]
A paper about allosteric as opposed to orthosteric binding to CB
receptors.
https://molpharm.aspetjournals.org/content/94/1/743
[1943]
"Studies have emphasized that gut microbiota modulates the
intestinal eCB system tone, which, in turn, regulates gut permeability
and plasma LPS, and is able to stimulate peripheral endocannabinoids
in the gut and adipose tissue. This hyperactivity of the CB1 receptor
increases the permeability of the gut barrier, favoring the
translocation of more LPS into the bloodstream, which will further
stimulate the eCB system, generating a cycle in which both remain
altered. In adipose tissue, eCB disturbance leads to adipogenesis,
contributing to the accumulation of body fat and, consequently,
obesity. LPS and eCB regulate, in different ways, the apelinergic
system in adipose tissue, reducing the secretion of apelin and the
expression of its AP1 receptor. The apelinergic system plays a role in
energy and glycemic homeostasis. Thus, gut microbiota seems to play a
significant role in controlling the endocannabinoid system and,
consequently, as modulators of obesity and energy
homeostasis."
"In a mice model, it was observed that increasing the percentage
of linoleic acid (18:2 n-6) in the diet led to increased levels of
2-AG and AEA, which are derived from arachidonic acid (20:4 n-6),
which, in turn, is formed from linoleic acid in the
body."
"dietary lipids can modulate eCB system tone."
https://www.intechopen.com/chapters/63663
[431]
Yap et al (2026) add some "In silico insights on the binding site
and function of cannabinoids and cannabinoid acids on human 5-HT1A
receptor", finding that
"CBD, CBG and CBGa are potential partial agonists of 5-HT1A
receptor.
CBD, CBG and CBGa may compete with orthosteric ligand for binding.
CBDa, THCV and THCVa are potential allosteric modulators of 5-HT1A
receptor.
CBDa, THCV and THCVa can block the exit of orthosteric ligand from its
binding site.
MD + 7TM Open IC can accurately predict the activity of 5-HT1A binding
ligands."
https://www.sciencedirect.com/science/article/pii/S1093326325002463
[5469]
However, and since we must allow alcoholics their freedom to drink,
excess gut permeability may be undesirable in the progression of liver
disease:
"Liver disease is often times associated with increased
intestinal permeability. A disruption of the gut barrier allows
microbial products and viable bacteria to translocate from the
intestinal lumen to extraintestinal organs. The majority of the venous
blood from the intestinal tract is drained into the portal
circulation, which is part of the dual hepatic blood supply. The liver
is therefore the first organ in the body to encounter not only
absorbed nutrients, but also gut-derived bacteria and pathogen
associated molecular patterns (PAMPs). Chronic exposure to increased
levels of PAMPs has been linked to disease progression during early
stages and to infectious complications during late stages of liver
disease (cirrhosis)."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4451427/
[432]
As, in the seventeenth year of the ZPPPD, Slovenia went from
pretending cannabinoids had no medical uses to pretending only one
cannabinoid had only one medical use, to carry on generating excuses
to confiscate people's money, protect big pharma, and churn profits
for its law businesses at the expense of drinkers' lives, Wang et al
(2017) showed in binge drinking mice that "Cannabidiol attenuates
alcohol-induced liver steatosis, metabolic dysregulation, inflammation
and neutrophil-mediated injury", explaining that:
"Herein, we investigated the effects of CBD on liver injury
induced by chronic plus binge alcohol feeding in mice. CBD or vehicle
was administered daily throughout the alcohol feeding study. At the
conclusion of the feeding protocol, serums samples, livers or isolated
neutrophils were utilized for molecular biology, biochemistry and
pathology analysis. CBD significantly attenuated the alcohol
feeding-induced serum transaminase elevations, hepatic inflammation
(mRNA expressions of TNFα, MCP1, IL1β, MIP2 and E-Selectin,
and neutrophil accumulation), oxidative/nitrative stress (lipid
peroxidation, 3-nitrotyrosine formation, and expression of reactive
oxygen species generating enzyme NOX2). CBD treatment also attenuated
the respiratory burst of neutrophils isolated from chronic plus binge
alcohol fed mice or from human blood, and decreased the
alcohol-induced increased liver triglyceride and fat droplet
accumulation. Furthermore, CBD improved alcohol-induced hepatic
metabolic dysregulation and steatosis by restoring changes in hepatic
mRNA or protein expression of ACC-1, FASN, PPARα, MCAD, ADIPOR-1,
and mCPT-1."
Note: mast cell protease 1 has no direct homolog in humans.
https://pmc.ncbi.nlm.nih.gov/articles/PMC6554654/
[5735]
De Ternay et al (2019) agreed CBD reduces hepatic alcohol
damage:
"CBD modulated the ethanol-induced dysregulation of numerous
genes and proteins involved in metabolism and liver steatosis, such as
key genes of fatty acid biosynthetic and oxidation pathway,
mitochondrial pathway, and transcription factor PPAR-α.
Furthermore, in the ethanol-fed mice group, CBD attenuated hepatic
neutrophils infiltration, oxidative and nitrative stress, decreased
several markers of liver inflammation such as TNF-α, the
expression of adhesion molecule E-selectin, proinflammatory chemokine
and cytokines, and thus, attenuated liver injury induced by chronic
plus binge ethanol exposure."
De Ternay et al review evidence in three areas of CBD benefit in AUD:
reduction of drinking, modulation the inflammatory processes in the
liver, and reduction of alcohol-related brain injury [ARBI].
Additionally, they say, CBD can reduce alcohol-related seizures,
anxiety, and chronic pain. [1921]
Erukainure et al (2021) stirred up further evidence by using whole
plant extracts to produce "Cannabis sativa L. (var. indica)
Exhibits Hepatoprotective Effects by Modulating Hepatic Lipid Profile
and Mitigating Gluconeogenesis and Cholinergic Dysfunction in
Oxidative Hepatic Injury":
"This study sought to investigate the hepatoprotective effect of
C. sativa on iron-mediated oxidative hepatic injury. Hepatic injury
was induced ex vivo by incubating hepatic tissues with Fe2+, which led
to depleted levels of reduced glutathione, superoxide dismutase,
catalase and ENTPDase [ecto-nucleoside triphosphate
diphosphohydrolase] activities, triglyceride, and high-density
lipoproteincholesterol (HDL-C). Induction of hepatic injury also
caused significant elevation of malondialdehyde, nitric oxide,
cholesterol, and low-density lipoproteincholesterol (LDL-C) levels
while concomitantly elevating the activities of ATPase, glycogen
phosphorylase, glucose-6-phosphatase, fructose-1,6-bisphosphatase,
amylase, and lipase. Treatment with the hexane, dichloromethane (DCM),
and ethanol extracts of C. sativa leaves significantly (p < 0.05)
reversed these levels and activities to almost near normal. However,
there was no significant effect on the HDL-C level. The extracts also
improved the utilization of glucose in Chang liver cells.
High-performance liquid chromatography (HPLC) analysis showed the
presence of phenolics in all extracts, with the ethanol extract having
the highest constituents. Cannabidiol (CBD) was identified in all the
extracts, while Δ-9-tetrahydrocannabinol (Δ-9-THC) was
identified in the hexane and DCM extracts only. Molecular docking
studies revealed strong interactions between CBD and Δ-9-THC with
the β2 adrenergic receptor of the adrenergic system. The results
demonstrate the potential of C. sativa to protect against
oxidative-mediated hepatic injury by stalling oxidative stress,
gluconeogenesis, and hepatic lipid accumulation while modulating
cholinergic and purinergic activities. These activities may be
associated with the synergistic effect of the compounds identified and
possible interactions with the adrenergic system."
https://pmc.ncbi.nlm.nih.gov/articles/PMC8724532/
[5737]
Gojani et al (2023) on the other hand took a reductive approach,
examining specific CCx:
"Our findings indicate that all five phytocannabinoids reduce
HG-HL-induced -cell loss likely through reducing apoptosis and
pyroptosis. The protective effects of CBD, THCV, CBC, and CBN were
seen in the GSIS impairment by HG-HL. Although all five
phytocannabinoids tested in this research demonstrated the capability
to inhibit β-cell dedifferentiation induced by HG-HL, CBD seems
to be more effective compared to the other phytocannabinoids, as
indicated by the specific biomarker responses of β-cells and
progenitor cells to CBD."
https://www.preprints.org/manuscript/202309.0973
[5736]
Walsh et al (2021) would like us to know that:
"Unlike the continuous cellular synthesis and storage of
neurotransmitters and neuropeptides, AEA and 2-AG are produced through
'on demand' cleavage of NAPE and PIP2. This provides for a temporal-
and localization-dependent release of the endocannabinoids (Lu and
Mackie, 2016). The actions of AEA and 2-AG are terminated following
their cellular uptake and degradation by intracellular hydroxylase
[fatty acid amide hydrolase (FAAH)] (for AEA) and lipase enzymes
(monoacylglycerol lipase) (for 2-AG). Therefore, drugs that inhibit
the cellular uptake of AEA and 2-AG or prevent their enzymatic
degradation should result in a potentiation of endocannabinoid
action."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8669157/ [854]
"Chemopreventive effect of the non-psychotropic phytocannabinoid
cannabidiol on experimental colon cancer" is the subject of a
2012 paper by Aviello et al when
"...we investigated its possible chemopreventive effect in the
model of colon cancer induced by azoxymethane (AOM) in mice. AOM
treatment was associated with aberrant crypt foci (ACF, preneoplastic
lesions), polyps, and tumour formation, up-regulation of phospho-Akt,
iNOS and COX-2 and down-regulation of caspase-3. Cannabidiol-reduced
ACF, polyps and tumours and counteracted AOM-induced phospho-Akt and
caspase-3 changes. In colorectal carcinoma cell lines, cannabidiol
protected DNA from oxidative damage, increased endocannabinoid levels
and reduced cell proliferation in a CB(1)-, TRPV1- and
PPARγ-antagonists sensitive manner. It is concluded that
cannabidiol exerts chemopreventive effect in vivo and reduces cell
proliferation through multiple mechanisms."
https://pubmed.ncbi.nlm.nih.gov/22231745/
[3685]
"Cannabidiol Targets Colorectal Cancer Cells via Cannabinoid
Receptor 2, Independent of Common Mutations" say Moniruzzaman et
al (2025):

"Our results demonstrate that CBD induces apoptosis and halts
proliferation, migration, and invasion of CRC cell lines in a
concentration-dependent manner. CBD showed potent antitumor effects in
the tested cell lines with no obvious effect from different mutations
such as KRAS, BRAF, APC, PTEN, etc. CBD also induced ER stress in CRC
cells but not in healthy intestinal organoids. Cotreatment with
SR144528 inhibited the effects of indicating involvement of CB2
receptor activation in the anticancer effects of CBD. Together, these
results demonstrated that CBD could be effective for CRC regardless of
the underlying mutation through CB2 receptor activation."
https://pubs.acs.org/doi/full/10.1021/acsptsci.4c00644
[3951]
Vago et al at the San Raffaele Scientific Institute, Milan have a
subheading in their paper entitled "The Mediterranean Diet as a
Source of Bioactive Molecules with Cannabinomimetic Activity in
Prevention and Therapy Strategy" (2022):
"Modulation of the ECS Alters the Microbiota Composition
"Recent studies have proven that targeting the ECS directly can
lead to an alteration in the composition of the gut microbiota in
favor of species with a positive impact on health. It was seen that
the microbiota and the endocannabidiome cooperate in a series of
intertwined pathways, which, when disrupted, can worsen preexisting
low-grade inflammation and insulin resistance in obese patients. The
involvement of CB1 in intestinal and metabolic homeostasis has been
studied in detail, identifying its antagonism as a possible way to
improve gut barrier function. A higher ECS tone has been associated
with an increase in gut permeability and treatment with a CB1 agonist
HU-210 induced, as a consequence, severe metabolic disturbances such
as glucose intolerance, lipid accumulation in the muscle and
endotoxemia. Bahrami et al. have proven for the first time that CB1
blockade improves colonic inflammation, systemic inflammation and
insulin resistance in diet-induced obesity (DIO) mice fed with a
high-fat diet and treated with Rimonabant (SR141716A), a CB1
antagonist. Interestingly, CB1 antagonist administration also altered
the gut microbiota composition in favor of more protective species
such as Akkermansia muciniphila, which is known to ameliorate DIO and
diabetes parameters such as endotoxemia, adiposity, glucose metabolism
and insulin resistance when transferred live in mouse models. This
species' abundance was suggested to be restored as a consequence of
increased expression of MUC2, a transcription factor in charge of host
mucin production regulation. Mucin is the main nutrient source for A.
muciniphila and is essential for its growth. These outcomes were
demonstrated to be rimonabant administration-dependent in obese mice
and were also proven to be independent from caloric restriction and
weight loss. In addition to increased abundance in A. muciniphila, the
authors observed a decrease in the Lachnospiraceae and
Erysipelotrichaceae families. This is a significant finding, as these
two bacterial families belonging to the Firmicutes phylum are thought
to be involved in weight gain and metabolic syndrome induction, but
also in diabetes and inflammation-related GI disorders. What appears
to make the link between CB1 antagonism and gut microbiota even
stronger is the increased production of butyric and propionic acid
evaluated by Bahrami et al. by conducting gas chromatography on the
mice's cecal material. This increased production of short chain fatty
acids can be explained by an increased abundance of beneficial
butyrogenic and propionogenic species following the administration of
Rimonabant. A. muciniphila is a prominent example of this statement,
as propionic acid is its main metabolite. This interpretation,
however, remains a hypothesis, as the authors believe the effects that
Rimonabant had on the composition of the gut microbial community in
toto could be secondary to its effect on the inflammatory state, which
then led to a change in the environmental characteristics of the
intestine."
They add:
"Markey et al. explored the impact of Candida albicans on the
gut-brain axis and its ability to dysregulate the balance of the ECS.
It has been seen that C. albicans colonization, while protecting the
gut's health against pathobionts, induces an AEA-CB1 deficit which
increases both stress-induced and basal corticosterone production
related to anxiety-like behavior. By administering a FAAH blocker
(URB597) to C. albicans colonized mice, the trend was reversed, while
no effect was noted in mock-colonized mice. K-means cluster analysis
supported the hypothesis that the AEA deficit was responsible for the
changes in behavior, which was further proven by the increased
abundance of two other NAEs (linoleoyl and linoleoyl ethanolamine) in
the cecum of C. albicans colonized mice. The authors explain that the
change in precursor abundance in the GI tract noticed through feeding
studies could contribute to the alterations in AEA levels that were
observed in this study. Despite not being involved in the
lifestyle-related diseases that are in study in this review, this is
an example of how there could be undiscovered links between certain
species of the microbial community and a healthier ECS equilibrium.
While Markey et al. showed that Candida albicans alone seems to have
the ability to modulate the ECS, Lacroix et al. showed that there is a
strong time-dependent association between the abundance of several
bacterial genera of the intestinal microbiota and the concentration of
AEA and 2-AG in the ileum and plasma of high-fat high sugar (HFHS)
diet-fed mice. This study also showed a decrease in CB2 expression in
the early stages of the HFHS diet, which could have shifted the ECS
mediator profile to preferential binding to CB1, which then increased
intestinal permeability, inflammation, insulin resistance and may have
led to a subsequent change in the composition of the microbiota. It is
undeniable that there are numerous undiscovered details that need to
be clarified by future studies, but these observations confirm that
there is some kind of cooperation between single microorganism species
that, each with its own metabolism, can contribute to a healthy gut
environment by acting on the ECS."
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC8839035/
[1014]
As Farooqi et al were to remind the medical profession in 2023 in the
context of endometriosis:
"Endocannabinoids and exogenous cannabinoids exert opposite
effects on gut permeability. For instance, when examining decreased
permeability as a result of inflammation, it was demonstrated that
2-AG and AEA increased permeability, while THC and CBD decreased
permeability." [5496]
Compare this to the state of knowledge fifteen years after General
Smuts' gift to the world, when there was no concept of lipids as
messengers. Chapter 46 of Bainbridge and Menzies' Essentials of
Physiology 9th edition (1940) "Intestinal Digestion and
Absorption" makes no special mention of gut commensals and the
process is treated as if a machine, almost without life. The most that
could be discerned about drug influences on peristalsis was that:
"Peristalsis continues in a normal fashion when all the nerves
passing from the central nervous system have been divided, but it is
abolished by painting the wall of the intestine with cocaine or
nicotine, which puts the myoneural plexuses of Auerbach and Meissner
out of action."
Bainbridge and Menzies' Essentials of Physiology 9th edition, 1940
[380]
But these were the Dark Ages of lipid biochemistry. The lipid
hypothesis became lost in the hedgerows:
"Nikolai Anitschkow that laid the foundation of what would later
be termed the lipid hypothesis, or the concept that elevated blood
cholesterol concentrations induced atherosclerosis. He showed that
feeding rabbits purified cholesterol raised blood cholesterol levels
and induced atherosclerotic lesion formation, and that the extent of
atherosclerosis was proportional to the absolute amount of and length
of exposure to high blood cholesterol. In contrast, similar
experiments in dogs and rats did not elicit a similar response,
results that lent skepticism to the lipid hypothesis. The inability to
induce atherosclerosis in these species was later found to be due to
their relative resistance to diet-induced
hypercholesterolemia."
https://www.jlr.org/article/S0022-2275(20)35387-6/fulltext
[1724]
Daniel Steinberg in a history of the cholesterol controversy
elaborates:
"Cholesterol feeding in these species [dogs and rats] failed to
induce lesions. So, understandably, these investigators concluded that
Anitschkows results must reflect some peculiarity of the rabbit. After
all, it is a strict herbivore that normally has zero cholesterol
intake and a very low fat intake. The rabbit model was dismissed as
irrelevant to human disease. What was not appreciated was the fact
that rats and dogs, unlike rabbits, are very efficient in converting
cholesterol to bile acids. Consequently, even on very high cholesterol
intakes the blood cholesterol in these species does not increase
appreciably."
and
"During World War II, Cohn et al. and Oncley, Scatchard, and
Brown at Harvard developed elaborate largescale methods for
fractionating human serum to provide materials useful in treating the
wounded. In the course of those systematic studies, they found that
the lipids of serum were concentrated in two major fractions having
α- and β-mobility, respectively."
To help us position the state of ignorance at this time in the
context of the conquest of cannabis, Steinberg goes on to explain that
at this time (i.e. after the League's last health investigation in
1935, after Reefer Madness came out (1936), after the Marijuana Tax
Act 1937, and after the war was over) as far as these major fractions
were concerned
"...nothing was known about their origin, their fate, or their
biological significance."
https://www.jlr.org/article/S0022-2275(20)31274-8/pdf
[1725]
What did the authors of the 1925 treaty and the 1961 SCND know about
the effects of cannabinoids on bile acids and
hypercholesteremia?
After some rather unpleasant experiments in dogs, in 1922 G. H.
Whipple of the School of Medicine and Dentistry, University of
Rochester, N. Y, writes:
"Evidently there is a mechanism in the normal animal which
controls the production and destruction of bile salts within certain
limits but this is a complete mystery."
https://journals.physiology.org/doi/pdf/10.1152/physrev.1922.2.3.440
[2045]
"In his seminal early paper (published in Dutch), [Cornelis] de
Langen described clinical relationships among diet, serum cholesterol,
and atherosclerosis: '. . . a cholesterol-rich diet and severe
metabolic diseases, such as diabetes, obesity, nephritis, and
arteriosclerosis, are associated with
hypercholesterolemia.'"
de Langen (1916) is credited with the first credible epidemiological
investigation of the role of cholesterol in atherosclerosis, although
it went mostly unnoticed. Similar findings seemed to confirm his
Diet-Heart theory in 1940.
http://www.epi.umn.edu/cvdepi/essay/cornelis-de-langen-diet-heart-theory-1916/
[2955]
Ancel Keys took the anti-fat crusade to town on behalf of the sugar
and carbohydrate industries. But the debate rages on, as experimental
design improved. For example "The fallacies of the lipid
hypothesis" by Uffe Ravnskov in the Scandinavian Cardiovascular
Journal, the author found as many or more than 50% of the relevant
studies showed:
"High cholesterol may be beneficial
By 1992, a meta-analysis of 19 cohort studies including more than 600
000 men and women from many countries had found that cholesterol was
inversely associated with mortality from respiratory and digestive
diseases, most of which were of an infectious origin. The observation
was in line with a large number of epidemiological, laboratory and
experimental studies showing that high cholesterol protects against
infections. The main effect seems to be exerted by the LDL
molecule."
https://www.tandfonline.com/doi/full/10.1080/14017430801983082
[2956]
In 2005 Mielke et al cast further doubt on the alleged evils of
cholesterol:
"Neuropsychiatric, anthropometric, laboratory, and other
assessments were conducted for 392 participants of a 1901 to 1902
birth cohort first examined at age 70. Follow-up examinations were at
ages 75, 79, 81, 83, 85, and 88. Information on those lost to
follow-up was collected from case records, hospital linkage system,
and death certificates. Cox proportional hazards regression examined
lipid levels at ages 70, 75, and 79 and incident dementia between ages
70 and 88.
"Results: Increasing cholesterol levels (per mmol/L) at ages 70
(hazard ratio [HR] 0.77, 95% CI: 0.61 to 0.96, p = 0.02), 75 (HR 0.70,
CI: 0.52 to 0.93, p = 0.01), and 79 (HR 0.73, CI: 0.55 to 0.98, p =
0.04) were associated with a reduced risk of dementia between ages 79
and 88. Examination of cholesterol levels in quartiles showed that the
risk reduction was apparent only among the highest quartile at ages 70
(8.03 to 11.44 mmol/L [311 to 442 mg/dL]; HR 0.31, CI: 0.11 to 0.85, p
= 0.03), 75 (7.03 to 9.29 mmol/L [272 to 359 mg/dL]; HR 0.20, CI: 0.05
to 0.75, p = 0.02), and 79 (6.82 to 9.10 mmol/L [264 to 352 mg/dL]; HR
0.45, CI: 0.17 to 1.23, p = 0.12). Triglyceride levels were not
associated with dementia."
https://www.neurology.org/doi/10.1212/01.WNL.0000161870.78572.A5?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200pubmed
[4788]
By 2023 the certainties of the previous century were undone. The
title "A short history of saturated fat: the making and unmaking
of a scientific consensus" speaks for itself.
Ignoring de Langen, it claims
"The diet-heart hypothesis was first proposed in the 1950s by
Ancel Keys".
and says
"The idea that saturated fats cause heart disease, called the
diet-heart hypothesis, was introduced in the 1950s, based on weak,
associational evidence. Subsequent clinical trials attempting to
substantiate this hypothesis could never establish a causal link.
However, these clinical-trial data were largely ignored for decades,
until journalists brought them to light about a decade ago. Subsequent
reexaminations of this evidence by nutrition experts have now been
published in >20 review papers, which have largely concluded that
saturated fats have no effect on cardiovascular disease,
cardiovascular mortality or total mortality. The current challenge is
for this new consensus on saturated fats to be recognized by policy
makers, who, in the United States, have shown marked resistance to the
introduction of the new evidence. In the case of the 2020 Dietary
Guidelines, experts have been found even to deny their own evidence.
The global re-evaluation of saturated fats that has occurred over the
past decade implies that caps on these fats are not warranted and
should no longer be part of national dietary guidelines. Conflicts of
interest and longstanding biases stand in the way of updating dietary
policy to reflect the current evidence."
Among the revelations by The Nutrition Coalition founder Nina
Teicholz:
"By the late 1960s, a bias in favor of the diet-heart hypothesis
was strong enough that researchers with contrary results found
themselves unable or unwilling to publish their results. For instance,
the largest test of the diet-heart hypothesis, the Minnesota Coronary
Survey, involving 9057 men and women over 4.5 years, tested a
diet of 18% saturated fat against controls eating 9%, yet did not find
any reduction in cardiovascular events, cardiovascular deaths, or
total mortality. Although the study had been funded by the NIH, the
results were not published for 16 years, after the principal
investigator, Ivan Frantz, had retired. Frantz is reported to have
said that there was nothing wrong with the study; We were just
disappointed in the way it came out. Frantz's decision not to publish
his results in a timely manner resulted in these contradictory data
not being considered for another 40 years."
and concludes
"Until the recent science on saturated fats is incorporated into
the U.S. Dietary Guidelines, the policy on this topic cannot be seen
as evidence-based."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9794145/
[2957]
Another revelation concerns the AHA:
"'The 1961 AHA advice to limit saturated fat is arguably the
single-most influential nutrition policy ever published, as it came to
be adopted first by the U.S. government, as official policy for all
Americans, in 1980, and then by governments around the world as well
as the World Health Organization.'"
...
"However, they were paid off to distribute this information. The
AHA accepted $20 million (in today's dollars) in funding from Procter
& Gamble, a corporation that conveniently makes and sells Crisco
Oil. The AHA recommended that everyone replace butter with 'heart
healthy' alternatives like vegetable oil or Crisco Oil."
...
"It's no wonder more people than ever are skeptical of public
health organizations and mainstream experts who claim to possess the
final word on health and nutrition, when there is so much proof that
information has been censored and even doctored in order to push a
certain message that will help corporations like Procter & Gamble
become richer and richer."
https://www.eviemagazine.com/post/american-heart-association-was-paid-procter-gamble-heart-disease-saturated-fat-seed-oils-sugar
[4490]
Joy Y Kiddie MSc, RD shared some 1976 handouts from Procter and
Gamble, who had tried to invent soap using waste cottonseed oil and
ended up inventing Crisco shortening, in 1911.


"Looking back on the role of fat manufacturers and the sugar
industry (outlined in the preceding article) on which foods were
recommended and promoted, it makes me question what I was taught and
who affected what I was taught. Given that it was known at the time
the sugar industry funded the researchers that implicated saturated
fat as the alleged cause of heart disease, I wonder what we dont know
about which industry funded which research. After all, the knowledge
about the sugar industry having funded the researchers that implicated
saturated fat only came out in November 2016 when it had occurred
decades earlier."
https://www.lchf-rd.com/2018/03/15/the-marketing-of-vegetable-oil-to-an-unsuspecting-public/
[4482]
The predilection amongst scientists to sail with the current was
prevalent.
Says Teicholz in a 2024 Medscape article:
"Recognizing the need for rigorous data, governments around the
world, including our own National Institutes of Health (NIH), spent
billions of dollars in the ensuing decades on some of the largest and
longest human clinical trials ever conducted. Somewhere between 10,000
and 53,000 people were tested on diets in which saturated fats were
replaced by unsaturated vegetable oils (the tally depends on which
trials are counted). However, the results did not turn out as hoped,
and so researchers, either unable or unwilling to believe the
outcomes, largely buried the data. For instance, the leaders of one
large NIH-funded study with findings unfavorable to the diet-heart
hypothesis did not publish them for 16 years. When asked why, one
reportedly replied that there was nothing wrong with the study; 'We
were just disappointed in the way it turned out.'"

https://www.medscape.com/viewarticle/882564?form=fpf#vp_5
[4481]
We are left wondering why, after decades of Proctor and Gamble's
advice via the auspices of the American Heart Association, to avoid or
reduce saturated fat, the average person is fatter than ever
before.
Yet for the Huntley College of Agriculture, California State
Polytechnic University, Pomona, "cholesterol is bad" was
still an article of faith in 2020.
https://www.mdpi.com/2072-6643/12/8/2329/pdf?version=1596540267
[2958]
While in 2021 the e-Journal of Cardiology Practice does not question
Ancel Keys' work, and takes a pretty uncritical view of the missteps
of the past. But does provide details of other contributors to the
discovery timeline, dietary debates and drug treatments. Several
iterations of lipid profile modelling culminated in the US 1998
guidelines which became the "gold standard" for
diagnosis.
https://www.escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-19/history-in-medicine-the-story-of-cholesterol-lipids-and-cardiology
[2960]
Does it sound to you as if the role of cholesterol in atherosclerosis
was settled at the time of the 1924/25 Conference?
How about by the time of the 1961 SCND?
And by the time of the 1971 Protocol, was it settled?
And when Slovenia inherited what it believed to be the drug treaty
obligations of the former Yugoslavia (however translated) in 1991, was
the cholesterol question satisfactorily resolved?
When the ZPPPD was enacted in 2000, was it settled then? For your
information, "The fallacies of the lipid hypothesis" was
published in 2009.
The attendees at these various measures wouldn't have known if
cannabis contributed in any way, perhaps positively, to the regulation
of bile salts?
Do you expect there is any evidence the Plenipotentiaries considered
that at all?
By the time cannabis was dropped from the British Pharmacopoeia in
1932, work was afoot to find out what these bile acids were. In 1934
Rosenheim and King applied the studies of Bernal (1932) to elucidation
of the structure of bile acids. Bile acids contribute to the digestion
of exogenous fats, e.g. triglycerides. With Wieland and Windaus'
formula of 1928
"...it seemed as if the last chapters in the story of one of the
most brilliant researches of organic chemistry had been written. The
ring system of an important group of natural subsyances had been
established with a degree of certainty which seemed to be
final."
But two carbon atoms remained "homeless" and
"It soon became apparent that the C2H5 group was not in Ring IV,
and in spite of four years' systematic effort it proved to be
impossible to place the two carbon atoms elsewhere in the ring system.
The old formula thus became untenable."
https://www.annualreviews.org/doi/pdf/10.1146/annurev.bi.03.070134.000511
[2044]
So could the authors of the Opium Treaty known anything about
cannabis and bile acids in 1925? Could the Kingdom of Yugoslavia have
known on the 6 January 1929?
Clearly if they did not know what the bile acids were, what their
structure was, and did not know what the active principles of cannabis
were, they could not have predicted the results of their interaction,
could they?
Once cannabis was banned, it couldn't be the object of respectable
research, could it?
In 1956 J B Carey
"...identified chenodeoxycholic acid (CDCA) as a major biliary
bile acid and proposed that lithocholic acid, its bacterial
metabolite, caused liver injury in man."
"When a meal is ingested, the hormone cholecystokinin is
released from the small intestine. Cholecystokinin induces gallbladder
contraction as well as relaxation of the valve (sphincter of Oddi) at
the end of the common bile duct where it empties into the small
intestine. Bile then enters the duodenum. Some of the bile acids are
absorbed in the jejunum, but most are transported by intestinal
peristalsis to the distal ileum where they are efficiently absorbed.
The bile acid molecules pass through ileal enterocytes and enter
portal venous blood to return to the liver. One of the early
illustrations of the enterohepatic circulation of bile acids with
values for man was presented by Sune Bergstrm in 1959 and is shown in
Fig. 8."
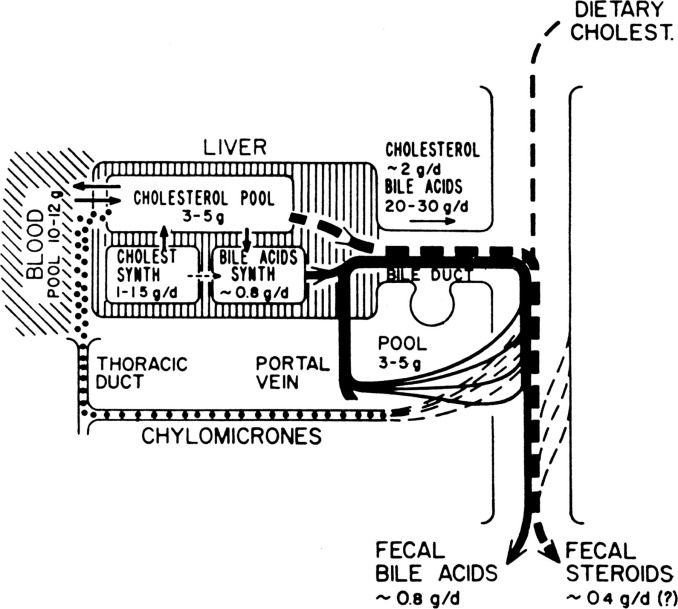
Now we've seen cannabis was widely used for antiemesis and digestive
assistance in the UK from its arrival with O'Shaughnessy in the 1840s
until its banishment after WW1.
Is there any way, in 1925, that the authors of the first
international drug treaty to include cannabis, knew anything about the
values for man for enterohepatic circulation of bile acids first
revealed by Bergstrm in 1959?
In his "Key discoveries in bile acid chemistry and biology and
their clinical applications: history of the last eight decades"
(2014) Hofmann and Hagey of the Department of Medicine, University of
California, San Diego, San Diego, CA reveal that
"The first symposium devoted solely to bile acids was organized
by Leon Schiff, a clinical hepatologist, who was one of the founders
of the American Association for the Study of Liver Diseases. This
symposium, held in 1967, was quite exciting for its participants who
are shown in Fig. 1."

"However, it is safe to say that the study of bile acids was
pursued by only a small number of laboratories, some in Departments of
Biochemistry and some in Departments of Medicine. Erwin Mosbach, one
of the early workers in bile acid metabolism, once stated to his wife,
'Whenever I go to the podium to give a paper on bile acids, everyone
leaves the room'.
"In 1965, the senior author, working in the laboratory of E. H.
Ahrens, began feeding studies with cholic acid in a patient with
severe hypercholesterolemia, and showed that cholic acid feeding was a
potent suppressor of bile acid and cholesterol biosynthesis, based on
measurement of fecal bile acids and sterols, using the newly developed
gas chromatographic method for fecal bile acids that had been
developed in this laboratory. It was logical to test CDCA, the other
primary bile acid, but at that time, the world's supply of pure CDCA
was thought to be less than 10 g, and the synthesis from cholic acid
was difficult. However, in the 1960s, a small English pharmaceutical
company (Weddell Pharmaceuticals) began the manufacture of CDCA for
unknown reasons. A kilogram was purchased for the senior author by the
Mayo Clinic in 1967. Leslie Schoenfield returned to the Mayo Clinic in
1966 after having spent a year in the laboratory of Sjvall, and
initiated a clinical trial with his fellow, Johnson Thistle, to test
whether oral cholic acid or hyodeoxycholic acid would lower
cholesterol in bile and ultimately induce cholesterol gallstone
dissolution. The senior author persuaded Schoenfield to add CDCA to
his protocol, and this study of Thistle and Schoenfield showed that
CDCA feeding decreased biliary cholesterol saturation, whereas neither
cholic acid nor hyodeoxycholic acid had any effect. In 1972, the first
gallstone dissolution induced by the ingestion of CDCA was observed,
initially at the Mayo Clinic, and later in London by a group led by
Hermon Dowling. [This was not the first time that the efficacy of oral
bile acids had been tested at the Mayo Clinic. In 1938, Philip Hench
had fed a mixture of conjugated bile salts in an unsuccessful attempt
to treat rheumatoid arthritis.]
"The discovery that CDCA [chenodeoxycholic acid] would induce
gradual dissolution of cholesterol gallstones led to the next
resurgence of interest in bile acids. For the very first time, CDCA
was made in kilogram quantities by several manufacturers, and became
the third bile acid available as a fine chemical."
https://www.sciencedirect.com/science/article/pii/S0022227520353232#bib34
[2042]
So would you agree that the authors of the international treaties of
1925 and 1961 did not know anything at those times about interactions
between cannabis and bile acids?
We can observe, in fact, that the human diet has undergone its most
dramatic modifications in the last 80 years. Ultraprocessed food,
starting in the nineteenth century, developed further after the war
with the wider entry of women into the workplace and the availability
of home refrigeration and, later, microwaves.
Some say ultra-processed food - this does have a strict scientific
definition - overtook smoking as the world's leading cause of death in
2019.
"The food system we live within is incredibly violent to our
bodies," says Chris van Tulleken, "and it desperately needs
changing. And people can't make choices that are healthy, many people
are incredibly constrained by the world around them."
And the doctor says:
"Food made by massive companies with obligations to pension
funds affects your body differently to food made at home by someone
that loves you. It's what we've all believed for decades, now we have
very robust evidence that proves it."
https://www.youtube.com/watch?v=l3U_xd5-SA8
[2668]
A prospective study with 105 159 participants examined
"Ultra-processed food intake and risk of cardiovascular disease:
prospective cohort study (NutriNet-Sant)" (2019) and here is the
graphical version of their findings.

"In this large observational prospective study, higher
consumption of ultra-processed foods was associated with higher risks
of cardiovascular, coronary heart, and cerebrovascular
diseases."
https://www.bmj.com/content/365/bmj.l1451
[2669]
"Ultra-processed food consumption, cancer risk and cancer
mortality: a large-scale prospective analysis within the UK
Biobank" in the Lancet (2023) found similar results.:
"The mean UPF consumption was 22.9% (SD 13.3%) in the total
diet. During a median follow-up time of 9.8 years, 15,921 individuals
developed cancer and 4009 cancer-related deaths occurred. Every 10
percentage points increment in UPF consumption was associated with an
increased incidence of overall (hazard ratio, 1.02; 95% CI, 1.011.04)
and specifically ovarian (1.19; 1.081.30) cancer. Furthermore, every
10 percentage points increment in UPF consumption was associated with
an increased risk of overall (1.06; 1.031.09), ovarian (1.30;
1.131.50), and breast (1.16; 1.021.32) cancer-related
mortality."
https://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(23)00017-2/fulltext
[2667]
In a cohort study of 10,775 individuals followed for a median of 8
years, Goncalves et al (2022) found that consumption of UPF greater
than 19.9% of total daily calories was associated with a faster
decline in global cognitive performance and executive
function.

In particular, individuals with ultraprocessed food consumption above
the first quartile showed a 28% faster rate of global cognitive
decline and a 25% faster rate of executive function decline compared
with those in the first quartile.
https://jamanetwork.com/journals/jamaneurology/fullarticle/2799140
[5136]
Fructose is a cornerstone of the ultra-processed food industry and
humans have never consumed so much fructose throughout human
evolutionary history as they do today.
In 2009 Ross et al showed such a diet produces impairments in a rat
water maze model, revealing one possible reason Americans elected
Donald Trump twice:
"Over the past three decades there has been a substantial
increase in the amount of fructose consumed by North Americans. Recent
evidence from rodents indicates that hippocampal insulin signaling
facilitates memory and excessive fructose consumption produces
hippocampal insulin resistance. Based on this evidence, the present
study tested the hypothesis that a high fructose diet would impair
hippocampal-dependent memory. Adult male Sprague-Dawley rats
(postnatal day 61) were fed either a control (0 % fructose) or high
fructose diet (60 % of calories). Food intake and body mass were
measured regularly. After 19 weeks, the rats were given 3 days of
training (8 trials/day) in a spatial version of the water maze task,
and retention performance was probed 48 h later. The high fructose
diet did not affect acquisition of the task, but did impair
performance on the retention test. Specifically, rats fed a high
fructose diet displayed significantly longer latencies to reach the
area where the platform had been located, made significantly fewer
approaches to that area, and spent significantly less time in the
target quadrant than did control diet rats. There was no difference in
swim speed between the two groups. The retention deficits correlated
significantly with fructoseinduced elevations of plasma triglyceride
concentrations. Consequently, the impaired spatial water maze
retention performance seen with the high fructose diet may have been
attributable, at least in part, to fructose-induced increases in
plasma triglycerides."
Some background:
"A high fructose diet causes numerous pathological changes,
including oxidative stress, glucose intolerance, insulin resistance,
type 2 diabetes, liver disease, hypertension, and cardiovascular
disease (Busserolles, Gueux, Rock, Mazur, and Rayssiguier, 2002;
Elliott, Keim, Stern, Teff, and Havel, 2002; Hwang, Ho, Hoffman, and
Reaven, 1987; Montonen, Jarvinen, Knekt, Heliovaara, and Reunanen,
2007; Nandhini, Thirunavukkarasu, Ravichandran, and Anuradha, 2005;
Zavaroni, Sander, Scott, and Reaven, 1980). Furthermore, a study from
one of the present investigators showed that the damaging effects of a
high fructose diet extend directly to the brain (Mielke, Taghibiglou,
Liu, Zhang, Jia, Adeli, and Wang, 2005). Specifically, placing male
Syrian hamsters on a 60 % fructose diet for 6 weeks produced
hippocampal insulin resistance. This finding is particularly
significant given that the hippocampus is integral to many forms of
learning and memory (Ergorul and Eichenbaum, 2004) and that converging
lines of evidence indicate that neural insulin signaling facilitates
hippocampal-dependent memory (Park, 2001). For instance, extensive
evidence suggests that peripheral insulin resistance and type 2
diabetes are associated with deficits in hippocampal-dependent
declarative memory (Convit, 2005; Messier, 2005; Stewart and Liolitsa,
1999; Strachan, Deary, Ewing, and Frier, 1997; Zhao, Chen, Xu, Moore,
Meiri, Quon, and Alkon, 1999). Moreover, learning and memory of a
spatial water maze experience are correlated with activation of the
hippocampal insulin signaling pathway (Dou, Chen, Dufour, Alkon, and
Zhao, 2005; Zhao et al., 1999). Most importantly, direct infusions of
insulin into the hippocampus enhance performance in a variety of
memory tasks, and the memory-enhancing effects of hippocampal insulin
administration are not observed in diabetic rats (Babri, Gholamipour,
Rad, and Khameneh, 2006; McNay, Herzog, McCrimmon, and Sherwin, 2005;
Moosavi, Naghdi, Maghsoudi, and Zahedi Asl, 2006).
"Given that fructose is preferentially metabolized by the liver
into lipids (Havel, 2005; Topping and Mayes, 1971) and produces large
increases in plasma triglyceride (TG) concentrations (Basciano,
Federico, and Adeli, 2005; Havel, 2005; Kelley, Allan, and Azhar,
2004; Le, Faeh, Stettler, Ith, Kreis, Vermathen, Boesch, Ravussin, and
Tappy, 2006; Park, Cesar, Faix, Wu, Shackleton, and Hellerstein,
1992), a high fructose diet is analogous to a high fat diet in many
metabolic ways. Importantly, rats fed a diet high in saturated fatty
acids exhibit impaired performance on a number of
hippocampal-dependent memory tasks (Greenwood and Winocur, 1990; 1996;
McNay et al., 2005). Moreover, high fat diets produce insulin
resistance in the brain (Banas, Rouch, Kassis, Markaki, and
Gerozissis, 2008), and injecting TGs directly into the brain
ventricles impairs memory (Farr, Yamada, Butterfield, Abdul, Xu,
Miller, Banks, and Morley, 2008). Collectively, the reviewed evidence
led us to hypothesize that a high fructose diet would impair
hippocampal-dependent memory, and that the deficits would be
attributable, at least in part, to fructose-induced increases in
plasma TGs. Consequently, the present experiment tested the effects of
feeding rats a high fructose diet on hippocampaldependent spatial
water maze learning and memory, and sought to determine whether any
deficits would be correlated with fructose-induced increases in plasma
TGs."
https://europepmc.org/backend/ptpmcrender.fcgi?accid=PMC2737072&blobtype=pdf
[3667]
Such ingredients are all but impossible to avoid in today's society
if you want to live a more-or less normal life. More efficient use of
food value may be one of the most valuable (subliminal) positive
outcomes, since food availability has grown immensely during the last
century, but nutritional content has fallen just as
dramatically.
According to Workinger et al in "Challenges in the Diagnosis of
Magnesium Status" (2018)
"Many fruits and vegetables have lost large amounts of minerals
and nutrients in the past 100 years with estimates that vegetables
have dropped magnesium levels by 8090% in the U.S. (Figure 2) and the
UK [cited include USDA ]. It is important to note that the USDA
mineral content of vegetables and fruits has not been updated since
2000, and perhaps even longer, given that the data for 1992 was not
able to be definitively confirmed for this review. The veracity of the
mineral content to support the claim of demineralization of our food
sources should be verified, particularly since farming methods and
nutrient fertilization has undoubtedly advanced in the last 50
years."

https://www.mdpi.com/2072-6643/10/9/1202
[2795]
"Magnesium is a cofactor in >300 enzymatic reactions.
Magnesium critically stabilizes enzymes, including many ATP-generating
reactions. ATP is required universally for glucose utilization,
synthesis of fat, proteins, nucleic acids and coenzymes, muscle
contraction, methyl group transfer and many other processes, and
interference with magnesium metabolism also influences these
functions. Thus, one should keep in mind that ATP metabolism, muscle
contraction and relaxation, normal neurological function and release
of neurotransmitters are all magnesium dependent. It is also important
to note that magnesium contributes to the regulation of vascular tone,
heart rhythm, platelet-activated thrombosis and bone
formation."
And their Table 3 lists a few of the enzyme functions...
Kinases B
Hexokinase
Creatine kinase
Protein kinase
ATPases or GTPases
Na+ /K+-ATPase
Ca2+-ATPase
Cyclases
Adenylate cyclase
Guanylate cyclase
Direct enzyme activation
Phosphofructokinase
Creatine kinase
5-Phosphoribosyl-pyrophosphate synthetase
Adenylate cyclase
Na+/ K+-ATPase
...membrane functions...
Cell adhesion
Transmembrane electrolyte flux
...as a calcium antagonist...
Muscle contraction/relaxation
Neurotransmitter release
Action potential conduction in nodal tissue
...and with structural functions in...
Proteins
Polyribosomes
Nucleic acids
Multiple enzyme complexes
Mitochondria
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4455825/
[2796]
The Defendant therefore believes that the nutritional quality of
mass-produced foods has declined as the quantity has increased, and
that this is not against the interests of the producers. Indeed isn't
the western deity of all our beverages full of empty calories?

As Lieber points out:
"Nutritional approaches can help prevent or ameliorate alcoholic
liver disease. For example, a complete balanced diet can compensate
for general malnutrition."
and
"Pure alcohol provides approximately 7.1 kilocalories per gram
(kcal/g), compared with 4 kcal/g for carbohydrates. Thus, a 12-oz can
of beer contains approximately 100 calories.
"At least under certain conditions, however, alcohol-derived
calories when consumed in substantial amounts can have less biologic
value than carbohydrate-derived calories, as shown in a study in which
Pirola and Lieber (1972) compared the weights of two groups of
participants who received balanced diets containing equal numbers of
calories. In one of the groups, 50 percent of total calories was
derived from carbohydrates, whereas in the other group the calories
were derived from alcohol.
"Although all participants received the same number of calories,
those in the alcohol group exhibited a decline in body weight compared
with those in the carbohydrate group. Moreover, when the participants
received additional calories in the form of alcohol, they did not
experience any corresponding weight gain. This suggests that some of
the energy contained in alcohol is 'lost' or 'wasted'that is, it is
not available to the body for producing or maintaining body mass.
Under other conditions, however, alcohol-derived calories have the
same biologic value as calories derived from other nutrients. The
various mechanisms involved and the circumstances in which alcohol
calories fully count or do not count are described in detail elsewhere
(Lieber 1991a).
"Several mechanisms have been implicated in the apparent loss of
alcohol-derived energy (Feinman and Lieber 1998). For example, some of
the energy may be used up (wasted) during the breakdown of alcohol by
a pathway known as the microsomal ethanol-oxidizing system (MEOS).
(For more information on this system, see the section 'Relationships
Between Nutritional Factors and Alcohol Metabolism,' below.) As
described later in this article, alcohol may damage the liver cells
mitochondriasmall membrane-enclosed cell structures that serve as the
cells power plantsand these damaged mitochondria may waste energy
during the breakdown of fats." [787]
In fact
"Researchers worldwide published a record 4,300+ scientific
papers on the subject of cannabis, according to the results of a
keyword search of the National Library of Medicine/PubMed.gov
website.
"This exceeds the total number of papers published during all of
last year [i.e. 2021], when scientists published over 4,200 papers. At
the time, that total was the highest number of cannabis-specific
papers ever published in a single year.
"Since 2010, scientists have published over 30,000 peer-reviewed
papers specific to cannabis, with the annual number of total papers
increasing every year. By comparison, researchers published fewer than
3,000 total papers about marijuana in the years between 1990 and 1999
and fewer than 2,000 total studies during the 1980s.
"'Despite claims by some that marijuana has yet to be subject to
adequate scientific scrutiny, scientists interest in studying cannabis
has increased exponentially in recent years, as has our understanding
of the plant, its active constituents, their mechanisms of action, and
their effects on both the user and upon society,' NORMLs Deputy
Director Paul Armentano said. 'It is time for politicians and others
to stop assessing cannabis through the lens of "what we dont
know" and instead start engaging in evidence-based discussions
about marijuana and marijuana reform policies that are indicative of
all that we do know.'"
https://norml.org/blog/2022/12/27/record-number-of-science-papers-published-about-cannabis-in-2022/
[2064]
In 1991, what did the Slovenian inheritors of the international drug
treaties of 1925, 1961 and 1971 know about the anti-emetic properties
of cannabis?
Let us take a note of the dates of some papers referred to
"Regulation of nausea and vomiting by cannabinoids and the
endocannabinoid system" from North American authors Sharkey et al
(2013):
"In clinical trials, cannabis-based medicines have been found to
be effective anti-emetics and even surpass some modern treatments in
their potential to alleviate nausea (Cotter, 2009; Tramr et al.,
2001). However, it was not until the early 1990s that the mechanism of
action of cannabis was established following the cloning of the
cannabinoid (CB) receptors (Howlett et al., 2002; Pertwee et al.,
2010). The significance of this discovery was enhanced when it was
realized that these receptors were part of an endogenous cannabinoid
(endocannabinoid) system in the brain and elsewhere in the body (Di
Marzo and De Petrocellis, 2012; Izzo and Sharkey, 2010; Mechoulam and
Parker 2013; Piomelli, 2003). The endocannabinoid system serves to
modulate the expression of nausea and vomiting when activated by
central or peripheral emetic stimuli (Darmani and Chebolu, 2013;
Parker et al., 2011)."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3883513/
[2043]
Does the Town Smell make me nauseous? I am not Slovenian, so
yes.
If you had asked any of the authors of these international drug
treaties, or the authors of the ZPPPD, about the effects of banning
cannabis for people affected by Ptuj Town Smell or other nauseating
experiences such as imbalances in microbiota caused by alcohol
consumption or undesirable ratios of exogenous lipids in foodstuffs on
the marketplace, they wouldn't have been able to refer to any of these
papers would they?
But what do you think they would have said if you had asked them?
If you had gone to them and said, look, we've got people feeling
queasy every time they go out of the house. We've got this Town Smell
in Ptuj and we just can't do without it. We just can't stop it, they
say, and you say why not. And they say "Because it's Ptuj."
So you say, well what about smoking cannabis to reduce the nausea and
also block out the smell seeping into your home? What would they say?
When the ZPPPD was introduced, would the authors have been able to
take into account results showing
"...that perturbation of bile acid homeostasis upon alcohol
exposure is mediated by activation of Cb1r and its downstream
effectors like phosphorylation of JNK signaling pathway and subsequent
activation of Crebh."
or
" that under normal conditions insulin plays a crucial role in
maintaining bile acid homeostasis via regulation of Crebh
transcriptional activity."
https://www.researchgate.net/publication/253336408_Hepatic_Cannabinoid_Receptor_Type_1_Mediates_Alcohol-Induced_Regulation_of_Bile_Acid_Enzyme_Genes_Expression_Via_CREBH/link/00b7d5200f5e64016f000000/download
[2046]
That was 2013. The experts you believe in already know about that in
1925, 1961 or 1971 or 1991 or when the ZPPPD was written in
1999?
And they couldn't have known in 1999 that
"Clearly, low doses of CB1 agonists (0.5 mg/kg Δ9-THC,
Limebeer and Parker, 1999; 0.0010.01 HU-210, Parker et al., 2003)
attenuate nausea in the conditioned gaping model, an effect that is
reversed by rimonabant (see Parker et al., 2011). At low doses (15
mg/kg, i.p.) the nonpsychoactive phytocannabinoid, CBD, also reduces
these nausea-induced behaviors (without affecting any measures of
motor activity) by its action as an indirect agonist of 5-HT1A
receptors in the dorsal raphe nucleus (Rock et al., 2012; Parker et
al., 2011). By acting as an agonist of the somatodendritic 5-HT1A
autoreceptors located in the dorsal raphe, CBD would be expected to
reduce the release of 5-HT in forebrain regions (e.g. possibly the
interoceptive insular cortex, Tuerke et al., 2012a) to ultimately
suppress toxin-induced nausea." [2043]
As the authors explain:
"These contextually elicited conditioned gaping or retching
reactions represent animal models of anticipatory nausea analogous to
that experienced by human chemotherapy patients, which can be produced
following 34 conditioning trials. In human chemotherapy patients, when
anticipatory nausea develops, the classic anti-emetic agent
ondansetron is ineffective in reducing this symptom (Hickok et al.,
2003); likewise rats and shrews pretreated with ondansetron do not
show a suppression of contextually-elicited gaping and retching
reactions, respectively (Limebeer et al., 2006; Parker and Kemp, 2001;
Parker et al., 2006; Rock et al., 2008). On the other hand, Δ9-
THC, URB597 and CBD all reduce these contextually-elicited conditioned
nausea reactions (Parker et al., 2011). More recently, it has been
shown that CBDA (Bolognini et al., 2012) were more potent than CBD and
Δ9-THC respectively in attenuation of contextually-elicited
conditioned gaping in rats. CBDA potently suppresses nausea and
vomiting in a 5-HT1A receptor dependent manner (Bolognini et al.,
2012). Since these compounds are both non-psychoactive, they are
promising candidates for the treatment of anticipatory nausea, as
there is no current therapeutic available once anticipatory nausea
does develop. Currently, patients are given non-specific anti-anxiety
drugs."
The authors do not explain why they think these psychoactive
properties are unwanted. They may be unwanted. Or they may be a bonus.
People do have the right to buy decaf and alkoholfrei also. The takeup
is not great.
It's not up to these researchers to decide people shouldn't be happy
as well as enjoying these particular benefits of, but not limited to,
CBDA, which by the way is not available as an anti-nausea drug in
Slovenia anyway, except as one of many useful components of
cannabis.
The authors seem happy to have discovered a component incapable of
making the patient happy. And the experts you believe in couldn't have
known that as of 2016 that
"The integrity of the gastric mucosa is maintained due to a
balance between mucosal aggressive factors and the so called gastric
mucosal protective mechanisms. The gastric mucosa is constantly
exposed to high concentrations of luminal acid. Other aggressive
factors in the lumen are pepsins, bile refluxed from incompetent
pyloric sphincter, bacteria, ethanol and drugs especially the
non-steroidal anti-inflammatory drugs (NSAIDs) capable of inhibiting
the synthesis of cytoprotective prostaglandins. The mucosa's ability
to withstand acid and other injurious agents is due to several
mechanisms collectively is known as the gastric mucosal barrier. The
mucus-bicarbonate layer together with surface-active phospholipids
barrier constitute the first line of defence or the pre-epithelial
barrier. The surface epithelial cells capable of rapid turnover and
migration (restitution) and releasing mucins, bicarbonate,
phospholipids, prostaglandins, trefoil peptides form the second line
of defence. Other important defence mechanisms of gastric mucosa are
cytoprotective prostaglandins, mucosal sulfhydryl content, adequate
mucosal blood flow, and sensory afferent innervations. The development
of gastric mucosa damage implies a breach in the balance between
aggressive and defencive factor."
They couldn't have known anything about the mechanisms by which
cannabis strengthens gastric mucosal defences?
"Several mechanisms are likely to account for the ability of
Cannabis or individual cannabinoid agonists to protect the stomach
against noxious injury. Cannabis and/or individual cannabinoids
inhibit gastric acid secretion, thereby, lessening the ability of this
most powerful aggressive factor to threaten the gastric mucosa.
Studies also indicated that Cannabis administration increases mucus
secretion in the gastric mucosa. Mucus is secreted by the mucous neck
and surface epithelial cells and plays an important role in protecting
the surface epithelial cells from luminal acid and other injurious
agents. Mucus retards diffusion of luminal acid into the mucosa and
together with bicarbonate secreted by the epithelium forms a pH
gradient with near-neutral pH at the surface of the mucosa.
"Luminal pepsins constitute an important aggressive factor
capable of digesting mucus and thereby increasing the susceptibility
of gastric mucosa to other injurious factors. Studies in
pylorus-ligated rats treated with Cannabis extract for 4 weeks
indicated that Cannabis did not affect basal pepsin secretion.
Cannabis, however, decreased pepsin secretion when the stomach is
stimulated with pentagastrin and carbachol. Cannabis also decreased
pepsin secretion following ethanol administration in rats.
"Reactive oxygen intermediates have been implicated in the
development of gastric mucosal injury due to ischaemia/reperfusion,
ethanol, NSAIDs, and bacteria. Cannabis has been shown to decrease
lipid peroxidation and to increase reduced glutathione content and
catalase activity in gastric mucosa. Cannabis also inhibited mucosal
nitric oxide. Although a vasodilator effect of physiological
concentrations of nitric oxide help the mucosa to withstand noxious
challenge, high concentrations are likely to have a damaging effect.
Cannabis thus might protect the gastric mucosa by virtue of an
antioxidant action.
"Mucosal inflammation plays an important role in the development
of gastric ulcers and although initial inflammatory response to the
gastric mucosa helps to minimize or limit tissue damage, an
exaggerated or uncontrolled response is detrimental to the mucosal
integrity. Cannabis has been shown to inhibit the pro-inflammatory
cytokine tumour necrosis factor-alpha in mucosal homogenates, an
action which might help to minimize the extent of mucosal
damage.
"Cannabis thus exerts antioxidant and anti-inflammatory effects
in the gastric mucosa. It is to be noted, however, that these actions
of Cannabis were evident only when the gastric mucosa was challenged
with increased acid secretion or after exposing the mucosa to noxious
agents such as acidified aspirin and ethanol and were not apparent
under basal conditions.
"One important factor in determining the ability of the gastric
mucosa to resist gastric acid and other noxious agents is gastric
mucosal blood flow. This has been inferred from studies showing that
interference with the blood supply to the mucosa i.e. ischaemia
resulted in the development of gastric mucosal damage or aggravated
the extent of mucosal damage evoked by NSAIDs or ethanol On the other
hand, agents which increase gastric mucosal blood flow such as
isoproterenol, vasodilator prostaglandins or capsaicin-type agents
helped to protect against noxious challenge. In this context, data
have been provided that the endocannabinoid anandamide increases
gastric mucosal blood flow. There is also an evidence for a
vaso-relaxant action for methanandamide in rat gastric arteries. This
effect was independent of cannabinoid receptors. It is thus possible
that a vasodilatory action is involved in the gastric protective
effects of Cannabis and or cannabinoids."
https://www.sciencedirect.com/science/article/pii/S1995764516300712#bib54
[2047]
So now you're a bit more up to date on the role cannabis can play in
these gastric mucosal protective mechanisms, at least up to May 2016,
do you say this has all been considered and taken into account in your
operations under the ZPPPD?
Now if cannabis helps gastric mucosal protective mechanisms, and
someone has some cannabis and Mr Teodorovic or the Police or the
Republic of Slovenia steal or confiscate someone's cannabis, or a
population's cannabis, what would you expect the effect would follow
from the removal of that cannabis on those gastric mucosal protective
mechanisms on that person or population?
In fact it would be worse for a population than a single person,
wouldn't it?
And there would be no difference between it being taken by a burglar
or by the government, would it?
Since 2016 how long have Slovenia's experts had to investigate these
negative effects of the ZPPPD on gastric mucosal protective
mechanisms?
And what evidence can you offer about these investigations?
What do you think the authors of the international drug control
treaties would have said at the time about cannabis and gut
motility?
Wasn't the British Empire pro-dysentery, pro-cholera, for the black
people?
Surely it would have been their own fault in colonial India? Would
they have tried cannabis to treat dysentery in white patients?
Staff Surgeon S J Rennie of the Cawnpore (now Kanpur) Hospital
reports unanimous success with treatment in a dozen or more such
individuals, reporting four of his case histories in detail in the
Indian Medical Gazette in December 1886 under the title "On the
Therapeutic Value of Tinctura Cannabis Indica in the Treatment of
Dysentery".
https://pmc.ncbi.nlm.nih.gov/articles/PMC5000962/
[4883]
General Smuts could not have known, could he, that as reported by
Izzo et al in the AGA journal Gastroenterology in 2003:
"Previous studies have shown that activation of enteric CB1
inhibits esophageal and gastrointestinal motility, including in
isolated human tissues, and in an experimental model of diarrhea in
the mouse. In this study, we were able to show that the nonselective
cannabinoid receptor agonist CP55,940 and the selective CB1 receptor
agonist ACEA decreased CT-stimulated fluid accumulation in the mouse
small intestine. The antidiarrheal effect of the cannabinoid agonists
examined here is very likely mediated uniquely by CB1 receptors
because: (1) the effect of both CP55,940 and ACEA was counteracted by
the selective CB1 receptor antagonist SR141716A; (2) the CB2 receptor
antagonist SR144528 did not modify the antisecretory effect of
CP55,940; (3) the CB1 selective agonist ACEA reduced CT-stimulated
fluid accumulation; and (4) the CB2 receptor agonist JWH-015 was
without effect."
https://www.gastrojournal.org/article/S0016-5085(03)00892-8/fulltext
[4884]
Statistics strongly supportive of an association between marijuana
use and improved gut motility can be found in a nationwide US survey
of 9645 adults 20-59 in 2019 by North Shore Medical Center, Salem,
Massachusetts and Massachusetts General Hospital, Boston:
"Recent MJ use was associated with a 30% decreased odds of
constipation (crude odds ratio: 0.71 [0.560.98], P = 0.005), which
persisted after stepwise adjustment for age and other demographic
factors including sex, ethnicity, education, body mass index, and
socioeconomic status (AOR: 0.64 [0.490.83], P = 0.001); comorbidities,
substance use (alcohol, tobacco, heroin, and cocaine), constipating
medications, general health condition, rigorous physical activity, and
emotional disturbances (AOR: 0.68 [0.480.93], P = 0.016); and diet
(AOR: 0.68 [0.520.89], P = 0.006). There was no association between
recent MJ use and diarrhea."
https://journals.lww.com/ajg/Abstract/2019/12000/Relationship_Between_Recreational_Marijuana_Use.15.aspx
[785]
In "The effects of D9 -tetrahydrocannabinol and cannabidiol
alone and in combination on damage, inflammation and in vitro motility
disturbances in rat colitis" (2010) by Jamontt et al at the
School of Life Sciences, University of Hertfordshire
"The 2,4,6-trinitrobenzene sulphonic acid (TNBS) model of acute
colitis in rats was used to assess damage, inflammation
(myeloperoxidase activity) and in vitro colonic motility.
Sulphasalazine was used as an active control drug.
"Key results: Sulphasalazine, THC and CBD proved beneficial in
this model of colitis with the dose-response relationship for the
phytocannabinoids showing a bell-shaped pattern on the majority of
parameters (optimal THC and CBD dose, 10 mg.kg(-1)). THC was the most
effective drug. The effects of these phytocannabinoids were additive,
and CBD increased some effects of an ineffective THC dose to the level
of an effective one. THC alone and in combination with CBD protected
cholinergic nerves whereas sulphasalazine did not.
"Conclusions and implications: In this model of colitis, THC and
CBD not only reduced inflammation but also lowered the occurrence of
functional disturbances. Moreover the combination of CBD and THC could
be beneficial therapeutically, via additive or potentiating
effects."
https://europepmc.org/backend/ptpmcrender.fcgi?accid=PMC2931570&blobtype=pdf
[2939]
In a murine colitis model, Yekhtin et al (2022) found
"Differential Effects of D9 Tetrahydrocannabinol (THC)- and
Cannabidiol (CBD)-Based Cannabinoid Treatments on Macrophage Immune
Function In Vitro and on Gastrointestinal Inflammation in a Murine
Model" and this was the Dextran sulfate sodium (DSS)-induced
colitis model. DSS is a sulfated polysaccharide. Administration of DSS
in mice causes human ulcerative colitis-like pathologies due to its
toxicity to colonic epithelial cells, which results in compromised
mucosal barrier function.
"...aimed to evaluate the effects of the phytocannabinoids D9
tetrahydrocannabinol (THC) and cannabidiol (CBD) on macrophage
activation. Macrophages from young and aged C57BL/6 mice were
activated in vitro in the presence of pure cannabinoids or cannabis
extracts. The phenotype of the cells, nitric oxide (NO) secretion, and
cytokine secretion were examined."
The treated mice did well and
"We identified higher activity of cannabis extracts as compared
with pure cannabinoids. Each treatment had a unique effect on cytokine
composition. Overall, our results establish that the effects of
cannabinoid treatments differ."
They explain
"Immunological dysregulation in IBD is characterized by
epithelial damage, expansion of inflammation driven by intestinal
flora, a large number of cells infiltrating into the lamina propria,
and a failure of immune regulation to control the inflammatory
response. In IBD patients, the number of macrophages increase in the
inflamed mucosa."
and
"Phytocannabinoids, the biologically active constituents of
cannabis, possess a wide range of immune regulatory properties,
mediated by the endocannabinoid system."
and as regards the two best known:
"D9 tetrahydrocannabinol (THC) and cannabidiol (CBD). THC and
some of the other phytocannabinoids mediate their biological effects
primarily through the classical cannabinoid receptors CB1 and CB2. In
addition, THC can act as an agonist of the receptors/channels GPR55,
GPR18, PPARγ, transient TRPA1, TRPV2, TRPV3, and TRPV4, and as an
antagonist of the receptors/channels TRPM8 and 5-HT3A. Interestingly,
although CBD affects the immune function, it has a very weak affinity
to CB2 or CB1, where it can act as a negative allosteric modulator.
Several reports have demonstrated that CBD acts as an agonist of other
receptors/channels, such as TRPA1, TRPV1, TRPV2, TRPV3, PPARγ,
and 5-HT1A, and as an antagonist of the receptors GPR55, GPR18, and
5-HT3A. CBD is also an inverse agonist of the receptors GPR3, GPR6,
and GPR12."
and again
"Cannabis extracts and pure cannabinoids were used in a
concentration of 5 g/mL; the extracts had stronger effect than the
pure cannabinoids, although cannabinoids constituted only 3538% of
their content. This could result either from inhibitory signaling of
other molecules in the plant (not THC/CBD) or from a synergistic
function of THC/CBD with other molecules."
and broadly their results showed
"Cannabinoid Treatments Reduce Nitric Oxide and Cytokine
Production of LPS-Activated Peritoneal Macrophages....Cannabinoid
Treatments Affect the Phenotype of Activated Peritoneal
Macrophages....Cannabis Extracts Have Improved Effect in Murine
Colitis DSS Model Mice as Compared with Pure
Cannabinoids....Cannabinoid Treatments Reduce Intestinal Macrophage
Infiltration and the Levels of Inflammatory Cytokines in the Plasma of
DSS Mice".
https://www.mdpi.com/2227-9059/10/8/1793/pdf?version=1658831384
[2938]
For Becker et al (2020) one model of colitis was not enough.
"Female C57BL/6 mice were treated with either cannabidiol [CBD],
Δ 9-tetrahydrocannabinol [THC], a combination of CBD and THC, or
vehicle, in several models of chemically induced colitis. Clinical
parameters of colitis were assessed by colonoscopy, histology, flow
cytometry, and detection of serum biomarkers; single-cell RNA
sequencing and qRT-PCR were used to evaluate the effects of
cannabinoids on enterocytes. Immune cell transfer from CB2 knockout
mice was used to evaluate the contribution of haematopoietic and
non-haematopoietic cells to colitis protection.
"Results: We found that THC prevented colitis and that CBD, at
the dose tested, provided little benefit to the amelioration of
colitis, nor when added synergistically with THC. THC increased
colonic barrier integrity by stimulating mucus and tight junction and
antimicrobial peptide production, and these effects were specific to
the large intestine. THC increased colonic Gram-negative bacteria, but
the anti-colitic effects of THC were independent of the microbiome.
THC acted both on immune cells via CB2 and on enterocytes, to
attenuate colitis."

"Conclusions: Our findings demonstrate how cannabinoid receptor
activation on both immune cells and colonocytes is critical to prevent
colonic inflammation. These studies also suggest how cannabinoid
receptor activation can be used as a preventive and therapeutic
modality against colitis."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8218712/
[2940]
From the Institute of Experimental and Clinical Pharmacology, Medical
University of Graz, a summary of important and recent findings on the
role of cannabinoid receptors and their ligands in the GI tract with
emphasis on GI disorders, such as irritable bowel syndrome,
inflammatory bowel disease and colon cancer:
"In ancient medicine, extracts of the marijuana plant Cannabis
sativa were used against diseases of the gastrointestinal (GI)
tract....After many anecdotal reports suggested beneficial effects of
Cannabis in GI disorders, it was not surprising to discover that the
GI tract accommodates and expresses all the components of the ECS.
Cannabinoid receptors and their endogenous ligands, the
endocannabinoids, participate in the regulation of GI motility,
secretion, and the maintenance of the epithelial barrier integrity. In
addition, other receptors, such as the transient receptor potential
cation channel subfamily V member 1 (TRPV1), the peroxisome
proliferator-activated receptor alpha (PPARα) and the G-protein
coupled receptor 55 (GPR55), are important participants in the actions
of CBs in the gut and critically determine the course of bowel
inflammation and colon cancer."

"The FAAH enzyme...seems to be a key molecule for the regulation
of endocannabinoid levels and colon motility, but not for GI pain
sensation."
"So far, the human studies indicate increased endocannabinoid
activity in colon cancer while the role of CB receptors remains less
clear.
"Cannabinoids reduce carcinogenesis in animal models of colon
cancer"
"The GI tract is one of the regions where cannabinoid signaling
is involved in many physiological and pathophysiological regulatory
mechanisms, this is now clearly understood."
"From a scientist's perspective and all the caveats in mind, it
seems to be a matter of time when cannabinoid compounds will be used
in the treatment of GI disease."
%20cannabinoids%20exert%20various%20anti-tumorigenic%20effects%20in%20colon%20cancer...see%20pic%20anti%20cancer%20effects%20433.jpg)
"A large number of studies have confirmed that the ECS is
crucially involved in the control of motility, secretion and mucosal
integrity of the gut and may even determine the course of intestinal
inflammation and cancer."
"From a scientist's perspective and all the caveats in mind, it
seems to be a matter of time when cannabinoid compounds will be used
in the treatment of GI disease."
Just hang on, they're saying. They might be able to agree with
something involving cannabis during my lifetime, just don't go doing
anything like treating yourself without them.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5130148/
[433]
And from a 2021 review:
"A database search of peer reviewed articles published in
English as full texts between January 1970 and April 2021 in Google
Scholar, MEDLINE, PubMed and Web of Science was undertaken. References
of relevant literature were searched to identify additional studies to
construct a narrative literature review of oncological effects of
cannabinoids in pre-clinical and clinical studies in various cancer
types.
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC8310855/
[5131]
In 2018 Ferro et al demonstrated a threefold increase in survival in
a mouse model of pancreatic cancer
"...inhibition of the G protein-coupled receptor GPR55, using
genetic and pharmacological approaches, reduces pancreatic cancer cell
growth in vitro and in vivo and we propose that this may represent a
novel strategy to inhibit pancreatic ductal adenocarcinoma (PDAC)
progression. Specifically, we show that genetic ablation of Gpr55 in
the KRASWT/G12D/TP53WT/R172H/Pdx1-Cre+/+ (KPC) mouse model of PDAC
significantly prolonged survival. Importantly, KPC mice treated with a
combination of the GPR55 antagonist Cannabidiol (CBD) and gemcitabine
(GEM, one of the most used drugs to treat PDAC), survived nearly three
times longer compared to mice treated with vehicle or GEM alone.
Mechanistically, knockdown or pharmacologic inhibition of GPR55
reduced anchorage-dependent and independent growth, cell cycle
progression, activation of mitogen-activated protein kinase (MAPK)
signalling and protein levels of ribonucleotide reductases in PDAC
cells. Consistent with this, genetic ablation of Gpr55 reduced
proliferation of tumour cells, MAPK signalling and ribonucleotide
reductase M1 levels in KPC mice. Combination of CBD and GEM inhibited
tumour cell proliferation in KPC mice and it opposed mechanisms
involved in development of resistance to GEM in vitro and in vivo.
Finally, we demonstrate that the tumour suppressor p53 regulates GPR55
protein expression through modulation of the microRNA
miR34b-3p."
https://www.nature.com/articles/s41388-018-0390-1
[1769]
THC was not tested in this paper.
"Cannabinoids in the landscape of cancer" by Mangal et al
(2021) presents in vitro and in vivo studies on pancreatic
adenocarcinoma:
"Phyto-, endogenous and synthetic cannabinoids demonstrated
antitumour effects both in vitro and in vivo. However, these effects
are dependent on cancer type, the concentration and preparation of the
cannabinoid and the abundance of receptor targets. The mechanism of
action of synthetic cannabinoids,
(−)-trans-Δ9-tetrahydrocannabinol (Δ9-THC) and
cannabidiol (CBD) has mainly been described via the traditional
cannabinoid receptors; CB1 and CB2, but reports have also indicated
evidence of activity through GPR55, TRPM8 and other ion channels
including TRPA1, TRPV1 and TRPV2.
"Cannabinoids have shown to be efficacious both as a single
agent and in combination with antineoplastic drugs. These effects have
occurred through various receptors and ligands and modulation of
signalling pathways involved in hallmarks of cancer
pathology."
https://link.springer.com/content/pdf/10.1007/s00432-021-03710-7.pdf#page=6.32
[786]
In 2019, a "Flavonoid Derivative of Cannabis Demonstrates
Therapeutic Potential in Preclinical Models of Metastatic Pancreatic
Cancer"
"This study reports on a new non-cannabinoid, non-psychoactive
derivative of cannabis, termed FBL-03G, with the potential to treat
pancreatic cancer. In vitro results show major increase in apoptosis
and consequential decrease in survival for two pancreatic cancer
models- Panc-02 and KPC pancreatic cancer cells treated with varying
concentrations of FBL-03G and radiotherapy. Meanwhile, in vivo results
demonstrate therapeutic efficacy in delaying both local and metastatic
tumor progression in animal models with pancreatic cancer when using
FBL-03G sustainably delivered from smart radiotherapy biomaterials.
Repeated experiments also showed significant (P < 0.0001) increase
in survival for animals with pancreatic cancer compared to control
cohorts.
https://www.frontiersin.org/articles/10.3389/fonc.2019.00660/full
[2413]
At the University of Camerino, Zeppa et al (2024) were less coy about
the magic ingredient of their pancreatic cancer treatment, with
"Cannabigerol Induces Autophagic Cell Death by Inhibiting
EGFR-RAS Pathways in Human Pancreatic Ductal Adenocarcinoma Cell
Lines":
"Immunoblots evidenced a decrease in EGFR expression in PANC-1
with the higher dose of CBG, while, for MIAPaCa-2, the reduction was
significant with both doses (Figure 2A). Similar results were obtained
for mTOR protein expression, which was reduced especially after the
treatment with the highest dose of CBG (Figure 2A). Then, total Akt
and its phosphorylated form were investigated. Data showed a slight
modulation of total Akt protein with CBG at a dose of 11.06 μg/mL
for PANC-1 cells and a reduction of phospho-Akt (pAkt) levels after
the administration of both CBG doses (Figure 2B). In MIAPaCa-2 cells,
the highest dose of CBG induced a marked reduction of total Akt and a
significant decrease in its phosphorylation (Figure 2B)."

https://www.mdpi.com/1422-0067/25/4/2001
[3979]
While Turgut et al (2022) found "Anti-cancer effects of
selective cannabinoid agonists in pancreatic and breast cancer
cells":
"We found that selective CB1/2 agonists suppressed cell
proliferation, clonogenicity and induced proapoptotic function in
human PANC1 pancreatic and MDA-MB-231 breast cancer cells. Based on
our findings, these agonists led to the inhibition of both cell
viability and clonogenic growth in a dose dependent manner. CB1/2
agonists were observed to induce intrinsic apoptotic pathway by
upregulating Bax, while downregulating Bcl-2 expression
levels."
https://www.elis.sk/download_file.php?product_id=7812&session_id=oh602ctcv1tfhp3l0hill6ql85
[4968]
In "Cannabinoids as Potential Therapeutic Agents in the
Treatment of Pancreatic Cancer" a review by Bimonte et al
(2025)...
"The search identified 46 studies, with 19 meeting the inclusion
criteria (14 preclinical and 5 clinical). Preclinical studies revealed
that cannabinoids, primarily Δ9‑ tetrahydrocannabinol (THC)
and cannabidiol (CBD), exert anti‑tumor effects through
mechanisms such as apoptosis induction, cell cycle arrest, inhibition
of angiogenesis, immune modulation, and reduction of oxidative stress.
Most clinical studies emphasize cannabinoids role in symptom
management rather than direct anti‑cancer effects. A notable
exception is a case series suggesting improved survival in pancreatic
cancer patients using CBD, though its preliminary findings warrant
further investigation."
https://ar.iiarjournals.org/content/anticanres/45/7/2719.full.pdf
[5130]
In 2021 Sultan et al showed the beneficial effects of anandamide
(AEA) - and by implication phytogenic THC - in lungs, colon and the
mesenteric lymph nodes experimentally infected with Staphylococcal
enterotoxin B (SEB).
"Upon analysis of vascular and gut leakage, we noted that
anandamide significantly decreased the leakage in the lungs (Figure
2D) and the gut (Figure 2E) in the SEB + AEA group, when compared to
the SEB + VEH group."
and
"To further investigate the effect of AEA on gut-associated
immune responses, we analyzed the effect of AEA on the mesenteric
lymph nodes (MLNs). The data showed that AEA significantly decreased
the percentage and absolute numbers of CD4 + T cells, CD8 + T cells,
Vβ8 + T cells, and NKT cells in the SEB + AEA group when compared
to the SEB + VEH group of mice (Figure 3AD)."
and
"Because we noted significant induction of AMPs [antimicrobial
peptides] following AEA treatment, we next investigated the microbial
profile in the lungs and the gut following SEB treatment. SEB
treatment increased the abundance of microbiota in the lungs, and AEA
significantly reversed this, as shown using Chao1 rare fraction
measure (Figure 5A). Beta diversity analysis, which measured the
similarity or dissimilarity between various groups, showed that all
three groups were well separated, with the SEB + AEA group clustered
away from the SEB + VEH group (Figure 5B). Additionally,
representatives of the orders of Caulobacterales and Pseudomonodales
were significantly decreased in the SEB + AEA group compared to the
SEB + VEH (Figure 5C,D). To distinguish significantly altered bacteria
among the three groups, linear discriminant analysis effect size
(LEfSe) analysis (Figure 6A) was performed and the corresponding
cladogram (Figure 6B) was generated. Data showed that there were
several bacteria found to be distinctly expressed in each of the three
groups. Our LEfSe analysis of the lungs indicated that beneficial
bacteria, such as Muribaculaceae (s24-7), was indicated in the SEB +
AEA group only. Additionally, some beneficial bacteria, such as
Lachnospiraceae and Clostridia which produce butyrate, were indicated
in the SEB + AEA group but not in the Nave or the SEB + VEH group.
Interestingly, some pathogenic bacteria such as Pseudomonas and
Enterobacteriaceae were indicated in the SEB + VEH group only but not
in the Nave or SEB + AEA."
https://www.mdpi.com/2073-4409/10/12/3305
[2710]
The Major Histocompatibility Complex (MHC) is the cellular machinery
that flags tumor cells for the immune system. However, most metastatic
tumor cells have lost their MHC expression, and thus escape immune
system killing. Dada et al (2022) set out an explanation of why
"Specific cannabinoids revive adaptive immunity by reversing
immune evasion mechanisms in metastatic tumours":
"Fascinating ethnographic and experimental findings indicate
that cannabinoids inhibit the growth and progression of several
categories of cancer; however, the mechanisms underlying these
observations remain clouded in uncertainty. Here, we screened a
library of cannabinoid compounds and found molecular selectivity
amongst specific cannabinoids, where related molecules such as
Δ9-tetrahydrocannabinol, cannabidiol, and cannabigerol can
reverse the metastatic immune escape phenotype in vitro by inducing
MHC-I cell surface expression in a wide variety of metastatic tumours
that subsequently sensitizing tumours to T lymphocyte recognition.
Remarkably, H3K27Ac ChIPseq analysis established that cannabigerol and
gamma interferon induce overlapping epigenetic signatures and key gene
pathways in metastatic tumours related to cellular senescence, as well
as APM genes involved in revealing metastatic tumours to the adaptive
immune response. Overall, the data suggest that specific cannabinoids
may have utility in cancer immunotherapy regimens by overcoming immune
escape and augmenting cancer immune surveillance in metastatic
disease. Finally, the fundamental discovery of the ability of
cannabinoids to alter epigenetic programs may help elucidate many of
the pleiotropic medicinal effects of cannabinoids on human
physiology."
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10010394/
[4659]
All of these discoveries were of course made up to eight decades
after the last medicolegal assessment of cannabis by the international
forces of prohibition (1935).
The Court will observe that if I wait as long as the United Nations
took to discover that weed isn't like heroin, for it to factor these
discoveries about what I have been doing to myself for the last 47
years into international law, by the time it percolates down to tell
Slovenia what the medical establishment wants it to do, I would be 123
years old before being able to legally obtain a longer, healthier
life, with less fat, better immunity, and less cancer.
Slovenia can be the country that fines people and drives them out of
their homes for refusing to be fat, less immune and more cancer-prone
if it wants to. This obviously puts this drug laws as currently
imagined in conflict with the Constitution and laws to protect the
person in health matters.
If people have to go to the ECHR to get their savings back from the
bank, or get compensated for losing their house over a 100 euro bill,
or as in the case of the erased, to establish their citizens' rights,
you can obviously expect a challenge sooner or later to this idea of
punishing the self-infliction of better health.
I'm not a member of a Christian death cult. I don't have any of the
things cannabis prevents, and like any reasonable person I will make
the choices required to keep it that way.
While all these discoveries were being made, prohibition continued in
its peaceful slumbers, and weed was still legally the same as
heroin.
----------------------------------------------------------------------------
The Englishman stands for the rights of everyone disadvantaged,
discriminated against, persecuted, and prosecuted on the false or
absent bases of prohibition, and also believes the victims of these
officially-sanctioned prejudices have been appallingly treated and
should be pardoned and compensated.
The Englishman requests the return of his CaPs and other rightful
property, for whose distraint Slovenia has proffered no credible
excuse or cause.
The Benedictions represent both empirical entities as well as beliefs.
Beliefs which the Defence evidence shows may be reasonably and
earnestly held about the positive benefits of CaPs at the population
level, in which the good overwhelmingly outweighs the bad. Below, the
latest version of this dynamic list.
THE BENEDICTIONS
REFERENCES
TIMELINE OF DRUG LAW v. SCIENCE













%20cannabinoids%20exert%20various%20anti-tumorigenic%20effects%20in%20colon%20cancer...see%20pic%20anti%20cancer%20effects%20433.jpg)
